Reviewed by Sahil Chopra, MD.
Research by Savit Malhotra and Theresa Do.
Introduction
As we continue our discussion of HRV and sleep, we will now turn our focus to a lesser-known aspect of sleep medicine: cyclic variation of heart rate (CVHR). To some, HRV and CVHR are analogous, but the differences between the two matter clinically. While a high HRV is typically associated with better overall cardiovascular health, the presence of CVHR during sleep reflects repeated disruptions in the body's autonomic nervous system, which is the system that automatically controls heart rate, breathing, and other vital functions. Although CVHR can be a powerful tool in understanding sleep health, it is often a lesser-discussed topic. By the end of this article, we hope that our readers will have a better understanding of CVHR and how it relates to HRV, as well as why HRV and CVHR could, when combined, give deeper insight into sleep health.
What is CVHR?
Cyclic variation of heart rate (CVHR) is defined as a distinct, repeating pattern of heart rate changes that occur during sleep.[1] This is especially true for individuals who have sleep-disordered breathing, such as obstructive sleep apnea.[2] In healthy young adults, heart rate drops by an average of about 24 beats per minute from waking levels, with smaller decreases in older adults (about 14 bpm).[3] During deep sleep (NREM), the nervous system shifts toward parasympathetic ("rest and digest") dominance, reducing heart rate, blood pressure, and cardiac workload.[4] However, in people with sleep-disordered breathing, this restful pattern is disrupted. During an apnea (a pause in breathing), the airway becomes blocked, and oxygen levels begin to fall. The body responds with what is known as the "diving reflex," where the vagus nerve slows the heart rate (bradycardia) while blood vessels constrict to preserve oxygen for vital organs.[3] When the brain senses the drop in oxygen and rise in carbon dioxide, it triggers a brief arousal that reopens the airway. At that moment, breathing resumes, the vagal brake is released, and a surge of sympathetic ("fight or flight") nervous system activity causes a rapid increase in heart rate (tachycardia) and a spike in blood pressure.[3] Essentially, the body fluctuates from a period of steady heart rate to a sudden cyclical sequence of slowing during an apnea to a rapid increase when breathing resumes.[5] This pattern, often ruled by the autonomic nervous system, repeats in cycles of hypoxia and arousal during an apneic event.[6]
While CVHR is the body's way of compensating for a lack of oxygen, it can lead to further issues down the line. For example, CVHR is often indicative that the body is undergoing some other form of physiological stress (such as sleep apnea or cardiovascular stress) that is disrupting sleep.[1] Additionally, one study has found that, in patients without ischemia (reduced blood flow causes reduced oxygen delivery to tissues), higher CVHR frequency was associated with worse diastolic function (reduced filling rates) and delayed ventricular relaxation (increased time to peak filling).[7] The same study also found that CVHR was independently associated with left ventricular diastolic dysfunction.[7] Over time, the underlying sleep-disordered breathing that produces CVHR is associated with serious cardiovascular consequences, including high blood pressure, heart rhythm disturbances, and changes in heart structure and function.[3] All of these point to the fact that CVHR, when left unacknowledged, can cause a host of cardiovascular issues.
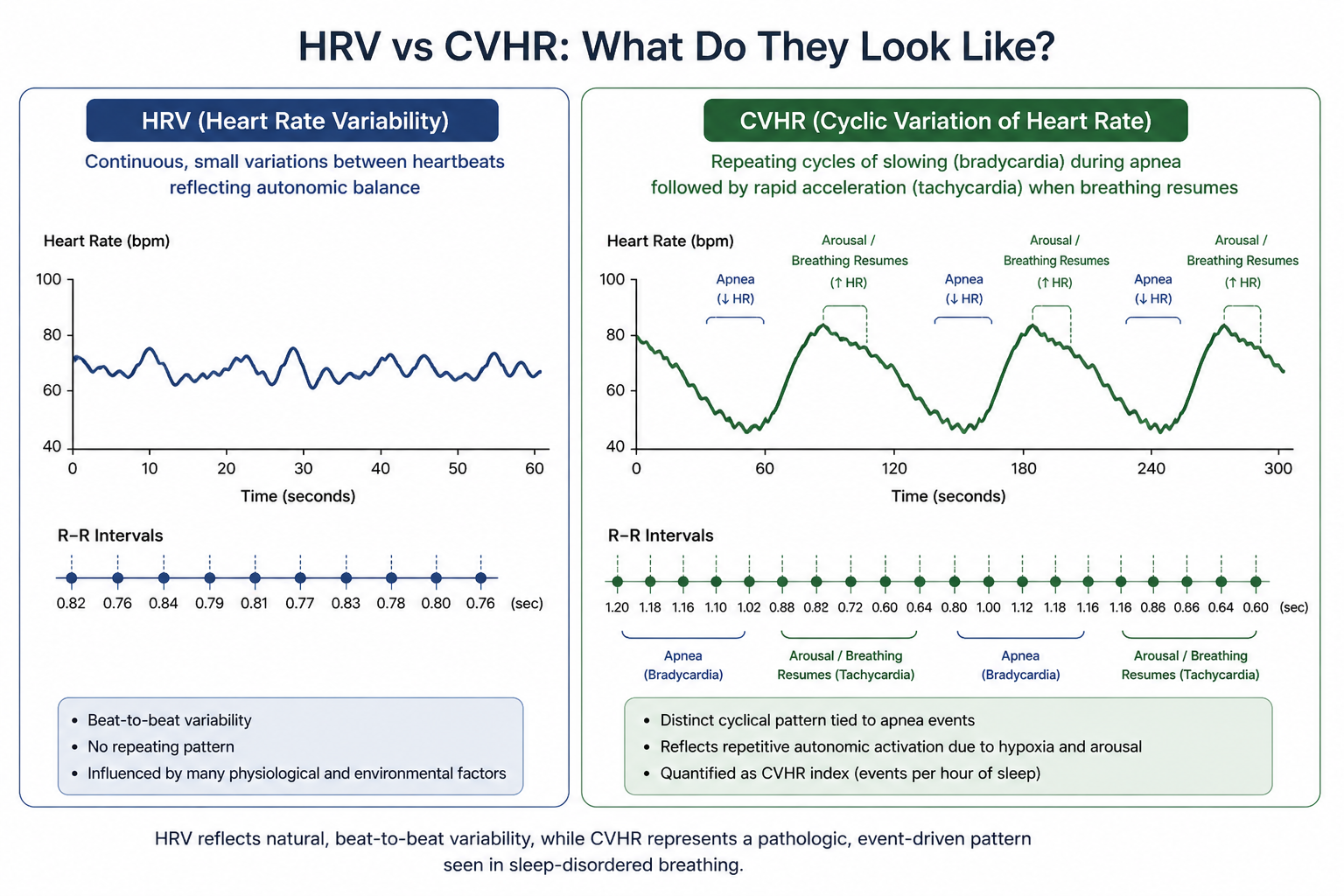
Key Differences Between HRV and CVHR
The key difference between heart rate variability (HRV) and CVHR lies in both what they measure and how clinically specific they are. As we have discussed previously, HRV is the measurement of the variation in time intervals between consecutive heartbeats.[8] It serves as an indicator of autonomic nervous system balance, combining both the sympathetic and parasympathetic inputs across many physiologic states (including stress, recovery, and sleep).[9] On the other hand, CVHR is a pattern of the heart rate, measuring the times during which the heart rate increases to feed more oxygen to the body.[10] Because CVHR is a measure of the heart rate during sleep, it serves as a targeted approach to better understand sleep-disordered breathing. While HRV is analyzed using time-domain and frequency-domain metrics over continuous recordings, CVHR is quantified as a period/percentage of the night spent having that cyclic heart rate pattern.[11,12] Many consumer-grade medical devices (such as the Apple Watch, OURA Ring, etc.) are able to derive an HRV value using built-in optical heart sensors (PPG) to determine inter-beat intervals or R-R intervals.[13] As for CVHR, this value often needs to be derived from ECG/PPG data during periods of sleep using a device like the SleepImage Ring System, or some other similar device.[1] These devices use sensors to measure oxygen desaturation (based on SpO2 values) and count the number of oxygen drops with corresponding heart rate.[1]
Limitations of HRV in Sleep and Why CVHR Matters
While HRV is a valuable indicator of autonomic system balance across various states, it has limitations when specifically assessing sleep health. HRV is non-specific compared to CVHR, as changes in HRV during sleep can stem from multiple physiological processes.[14] HRV combines both sympathetic (which speeds the heart up during stress) and parasympathetic inputs (which slow the heart down during rest), making it a broad measure of general cardiovascular health rather than a specific indicator of sleep-disordered breathing or sleep conditions. It is difficult to utilize HRV to pinpoint sleep issues, when it can be impacted by changes such as sleep stage transitions and thermoregulation.[15,16] For example, HRV naturally shifts as the body moves between lighter and deeper sleep stages, and it is also influenced by the body's temperature regulation processes that occur before and during sleep.[15]
In contrast, CVHR provides a more targeted measure since it takes into account by focusing specifically on the periodic heart rate fluctuations associated with sleep-disordered breathing events. Studies have shown that the CVHR index correlates closely with the apnea-hypopnea index, with a correlation of r = 0.84 in a study of over 860 patients, and it can identify moderate-to-severe sleep apnea with approximately 83% sensitivity and 88% specificity.[17] Notably, CVHR maintains its accuracy even in older adults and in people with reduced heart rate variability due to other conditions.[17] Therefore, while HRV offers a broad snapshot of overall autonomic health, CVHR provides a more focused and clinically actionable metric for identifying sleep-disordered breathing and its associated cardiovascular risks.
Conclusion
As we continue our discussion on HRV and sleep, it is important to understand the implications of CVHR so that the two are not confused. While they seem similar, HRV and CVHR differ drastically in terms of what they actually measure and their clinical significance. Nevertheless, both are incredibly useful when it comes to understanding your health. HRV provides a broad window into overall autonomic and cardiovascular health, while CVHR is a specific marker of sleep-disordered breathing and the autonomic disruption it causes. However, HRV can be impacted by sleep health, and poor CVHR outcomes could help your doctors understand why your HRV is not quite where you want it to be. In future articles, we will continue to explore this relationship between sleep and HRV, as well as where CVHR ties into the mix. If you are worried that your sleep may be impacting your HRV, we encourage you to find a healthcare provider to help you get back on track! The team here at Empower Sleep is always ready to help!